“Stay home. Break the chain of Transmission and save lives.”
In 2020, that is what New Zealand Prime Minister Jacinda Ardern asked all citizens to do, ‘unite’ and ‘lockdown’ to protect against the rapid spread of Covid-19.
This is not the first time an infectious disease has gripped the country, and it will not be the last according to Dr Mark Thomas who is an infectious disease specialist.
Dr Thomas believes Covid-19 came as a surprise to many, particularly as the rate of which it is spreading worldwide continues to rise.
“We have had influenza epidemics that have caused concern in the past.” says Thomas.
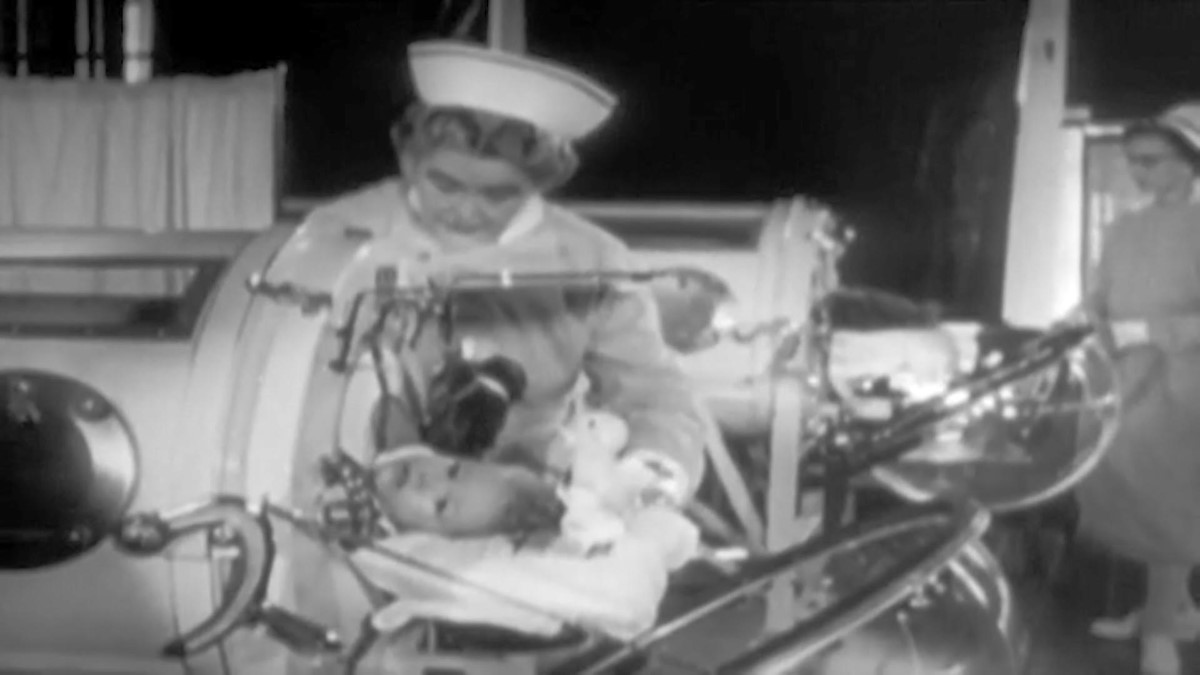
History shows us that infectious diseases used to be far more rampant in New Zealand than they are today. Diseases such as Polio, Measles and Meningitis for example, led to high rates of child death before vaccines were developed.
In recent years, New Zealand has experienced major outbreaks of Influenza, Measles, Mumps and Whooping cough, each of which have parallels with the Covid-19 outbreak.
The unprecedented Level 4 “Lockdown” (lasting 4 weeks - March to April 2020) required a “shift in thinking” from New Zealanders, according to Dr Nikki Turner, director of the New Zealand Immunisation Centre.
“It’s a shift away from individual issues to where we think about ourselves as a community.” Dr Turner believes.
Dr Turner believes that viruses don’t take an individual approach and therefore neither should humans.
“The viruses don’t go for the individual, they spread through the whole community.” She explains.
The ‘greater good’ is the overall message from leading health experts when it comes to enforcing tough measures like the nationwide lockdown in order protect the population.

Defeating Covid-19, is a confusing and frustrating task for many, as most New Zealanders have never had to worry about infectious diseases. Mostly because vaccines are available free of charge to all kiwis from birth.
No vaccine exists currently for Covid-19.
The virus jumped to humans from livestock less than 6 months ago and a vaccine is at least another 12 months away, which is cause for concern in terms of the transmission rate and the serious effects of the virus.
The Polio epidemic of the 1940’s and 1950’s stands out as one of the most devastating outbreaks in New Zealand’s medical history and can be used as a good example of the long-term effects of a pandemic which left thousands of children with lifelong paralysis. Over time a vaccine was developed, and today wide scale immunity protects against an outbreak of polio.
By the 1960s New Zealand’s public health service committed to an ongoing community wide vaccination programme, to give protection against a range of illnesses.
Dr Nikki Turner explains just how common infectious diseases were in New Zealand in the past.
“What New Zealand is unaware of is where we’ve come from. Infectious diseases used to be rampant, people lost their infants all the time, there were huge rates of child death. We improved considerably with better sanitation, better hygiene, better housing, and we got much better healthcare.” She says.
“However, infectious diseases continue to range in the NZ population.” she adds.
Dr Turner believes that overall, New Zealand is doing well with immunisation coverage.
“We used to be really bad about twenty to thirty years ago, we had really poor immunisation coverage, and we’ve improved really well over the last twenty years. So now we have around about 92-93% of our infants fully vaccinated, at times nearly up to 95%.” She explains.
The measles outbreak has been an ongoing challenge for health officials in New Zealand even though universal vaccination was introduced in 1969. The last two major measles epidemics in New Zealand occurred in the 1990s with thousands of cases, hundreds of hospitalisations and seven deaths.
Cameron Edwards contracted Measles at the age of 13. He was not immunised and the illness nearly claimed his life, leaving him with on-going health issues.
“When you see your incredibly healthy young man, lying there not knowing if whether he was going to live or not. It’s completely awful and you have no control, you’re in the hands of the doctors.” His mother Ally says.
“I’d never seen measles before. Of course, it wasn’t something that I had even considered to be a deadly infectious disease. But having been on the receiving end of a high-level reaction to it, it was really scary.”
Not immunising Cameron was a decision made by Ally after she had heard that it can cause disorders in children who have had the vaccine.
“I made the decision not to vaccinate Cameron for measles, mumps and rubella. That was based on research around at the time about it causing Autism. I wasn’t prepared to take that risk because it wasn’t something I wanted to expose my children to.” She recalls.
The family believed that Cameron was suffering from a form of Influenza. His symptoms were consistent with a bad case of the flu and they all believed he would eventually fight the illness off.
“He started to deteriorate further so I took him in to the GP. The doctor began checking him and I was extremely alarmed when I was instructed to get him to hospital, and that an ambulance would take too long”. Ally remembers.
Cameron didn’t realise how serious his situation was until multiple doctors showed up in his hospital room, dressed in protective equipment. The doctors were not only trying to help Cameron, but they were also learning about the virus from him.
“I couldn’t breathe much until they put oxygen on me and by then I was scared that I wouldn’t pull through.” He says.
Ally says she felt guilt towards not vaccinating her son but believes her reasons at the time were valid.
“There was a lot of guilt around that. Because I hadn’t revisited that research information.” She admits.
Measles has been an international scourge for thousands of years, and in a country without a vaccination program you get epidemics of measles every year.
Prior to a vaccination program nearly every child in the country catches measles.
“People say, ‘so what it’s not a big deal, they’ll then get immune.’ But for every child that gets measles, between one in a thousand, and one in two thousand will die, and around one in a thousand and one in two thousand will end up with significant brain damage.” Says Dr Nikki Turner.
In 2017, Dr Julia Peters and her team at Auckland Regional Public Health faced one of the worst outbreaks of Mumps in more than 30 years. It is highly contagious and affects the salivary glands but can lead to seizures and brain damage. The team spent months tracking and monitoring cases to contain the spread.
Dr Peters found that 75% of all cases in this outbreak were found to be among people who were either un-immunised or only partially immunised.
“Many of the people who came in with the mumps, many of them came from the Pacific where there were outbreaks of the mumps. It came into a vulnerable population and despite our best efforts it took hold.” She says
Every country in the world has a national vaccination program focused on numerous infectious diseases. The World Health Authority recommends this because the science behind vaccines, particularly the vaccines used in national vaccination programs, is overwhelming.
“Behind water, it is the strongest evidence of anything we do in medicine.” Peters says.
As with Covid-19, Whooping cough is an intense respiratory disease readily spread in the community by coughing and sneezing
Catherine and Greg Hughes lost their infant son Riley after contracting Whooping cough, the highly contagious respiratory disease that affects the lungs and airway.
The couple noticed their son wasn’t getting over the cough and it was only getting worse. They took him to hospital, but he showed little signs of improvement.
That’s when things got desperate for the family, Catherine explains.
“I started begging – ‘Can't you do a transplant!?’. I didn't want to think this was it, this was over. I remember watching the beeps. It kept getting slower and then he was gone.” She remembers.
In 2017 New Zealand’s Ministry of Health declared a national outbreak of whooping cough. One thousand three hundred and fifteen cases were reported.
Professor Anne La Flamme of Biological Sciences, Victoria University of Wellington views immunity as protection.
“You can think of it as politically when you have immunity from something – you have protection from that. For us it’s protection from disease causing organisms or pathogens, that’s our immunity. We don’t naturally have a specific immunity, but we have immune response that can allow us to develop that immunity.” She says.
However, she reveals that humans have another part of our immune system which can develop a specific recognition of a virus and remember it. The immune system can have memory, and by developing that memory it means that next time immune systems are exposed to something, they can react much more effectively.
“More efficiently than you would normally.” She says.
La Flamme explains how this has benefits to the people exposed to it.
“In that context that vaccine is giving you that first exposure, but it is a controlled exposure so that there’s no disease. One of the benefits of having an exposure is that you have that immunity, but you have to suffer the disease and nobody wants to suffer the disease. In a way, a vaccine is doing that because it is saying to your immune system ‘this is a dangerous organism you might see it again, and this is what you need to do to protect yourself.” She says.
Dr Nikki Turner says that pregnant women who decide to vaccinate themselves pass their immunity to their unborn children.
“You get a lot of protection from your mother, so now we recommend strongly vaccinating in pregnancy. As the mother gets good antibodies, she passes those to the infant before they are born. And that if we vaccinate mothers the new-born infants have very high levels of protection” She says.
The New Zealand strategy is to protect young infants against whooping cough and making sure the infants start their own immunisation programme on time. The last epidemic in New Zealand saw four young infants die as they were too young to begin immunisation.
As doctors and scientists monitor daily news about Covid-19, the world hopes and waits for a vaccine or cure for the virus and experts believe the horrifying experience of Covid-19 has given us all a clearer understanding of the ever-present threat of infectious disease.
There are potential options. One potential approach is using blood from people who have recovered from Covid-19 by using the antibodies in their blood, and passively offer it to someone else.
“None of them are here now (covid-19 vaccines), none of them are clear, and they would require a big scale up to be available. So that’s why the key message for all of us is if we can reduce the impact on our communities now and the impact on our healthcare services it gives us more time.” Says Dr Turner.
So this is not just about Covid-19. This is about keeping ourselves healthy as a community against other nasty infectious diseases that we do not want to see back.
Words by Mark Shaw


